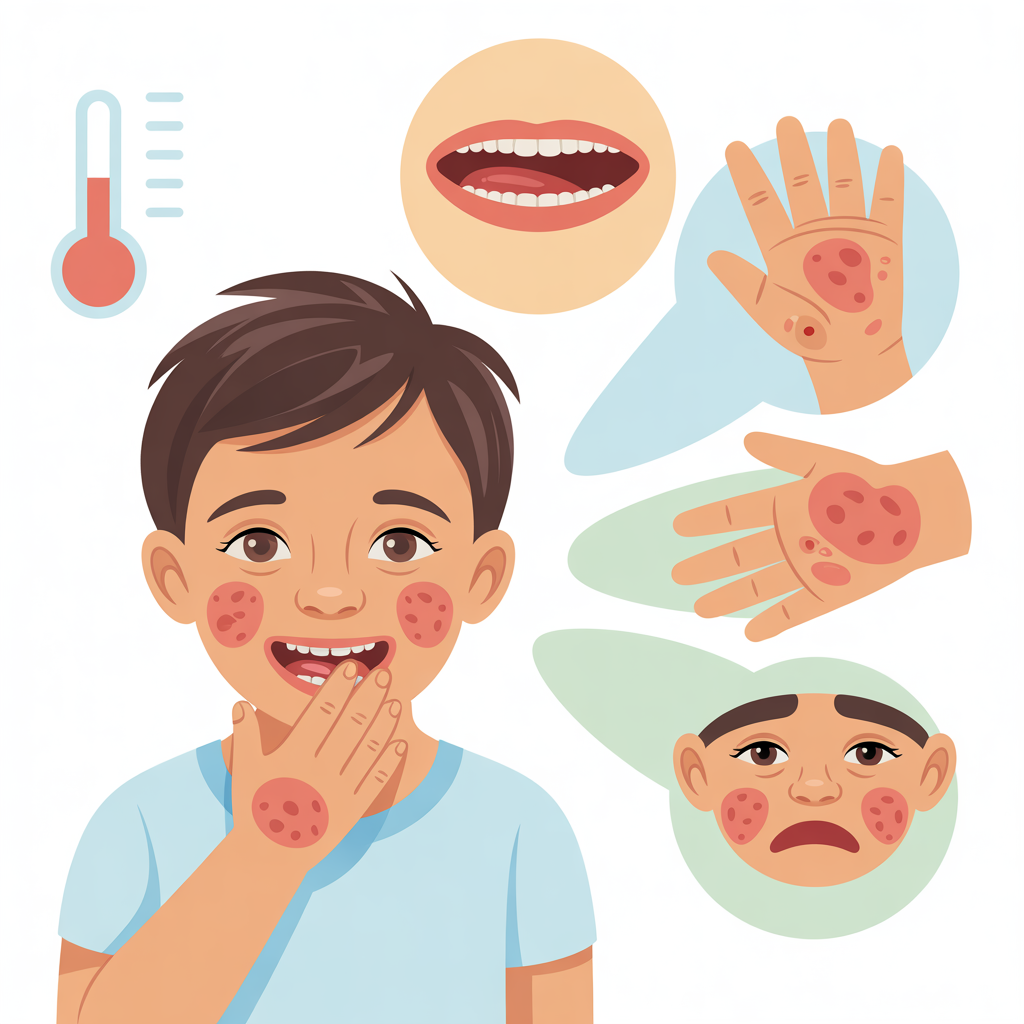
Hand, foot and mouth disease (HFMD) is a common contagious viral illness that primarily affects infants and young children under 5 years old — but it can also occur in older children and adults. Caused most often by the coxsackievirus A16 or enterovirus 71, this disease is known for its distinctive pattern of sores and rashes appearing in the mouth, on the hands, and on the feet. While it is usually mild and self-limiting, recognizing the symptoms early is essential for managing discomfort and preventing the spread to others. Below is a comprehensive breakdown of the most common — and sometimes overlooked — symptoms of hand, foot and mouth disease, from the very beginning of infection through each stage of the illness.
1. Sudden Fever
One of the earliest and most consistent signs of hand, foot and mouth disease is a sudden onset of fever. This is typically the first symptom to appear and can precede other visible signs by 1 to 2 days, making early diagnosis challenging.
- Temperature range: The fever usually ranges between 101°F (38.3°C) and 104°F (40°C).
- Duration: The fever typically lasts for 3 to 5 days.
- In children: Young children may become unusually irritable, cry more than usual, and appear lethargic or sluggish.
- In adults: Adults with HFMD may experience a lower-grade fever or sometimes no fever at all, making symptoms less obvious.
A sudden unexplained fever in a child who has been in contact with others recently — especially in a daycare or school setting — should prompt parents to watch for additional HFMD symptoms in the days that follow.
2. Sore Throat
Shortly after or alongside the fever, many individuals develop a sore throat. This symptom is caused by inflammation of the throat and the early formation of small blister-like lesions at the back of the mouth and throat.
- The throat may appear red and irritated even before visible sores develop.
- Children may refuse to eat or drink due to pain and discomfort when swallowing.
- The soreness can range from mild scratchiness to significant pain depending on the severity of the infection.
This symptom is especially important to monitor in young children, as refusal to drink fluids due to throat pain can quickly lead to dehydration.
3. Loss of Appetite
Due to the combination of a sore throat, painful mouth sores, and general feelings of illness, loss of appetite is a very common symptom of hand, foot and mouth disease. This occurs at the very beginning of the illness and can persist throughout its course.
- Children may refuse their favorite foods and drinks.
- Eating or drinking may become painful, particularly once mouth sores develop.
- Parents should offer cool, soft foods such as yogurt, applesauce, or cold water to help maintain nutrition and hydration.
- Avoid giving acidic foods (like orange juice or tomato-based products) as they can worsen mouth sore pain.
4. Painful Mouth Sores (Herpangina)
One of the hallmark symptoms of HFMD is the development of painful sores inside the mouth, a condition also referred to as herpangina. These sores typically appear 1 to 2 days after the initial fever and are one of the most distressing aspects of the illness, especially for young children.
- Appearance: Small, red spots that quickly develop into tiny blisters about 2 to 3mm in size, which then break open to form shallow, painful ulcers with a gray or white center and a red border.
- Location: They typically appear on the tongue, gums, inner cheeks, the roof of the mouth (palate), and the back of the throat.
- Number: There are usually between 3 and 10 sores, though more can develop.
- Pain level: The pain can be intense, making it very difficult for children to eat, drink, or even swallow saliva comfortably.
- Duration: These mouth sores typically last for 7 to 10 days before healing on their own.
Because these sores closely resemble those of other conditions (like cold sores), a doctor can help confirm whether they are indeed caused by HFMD.
5. Skin Rash on the Palms of the Hands
The skin rash on the hands is one of the defining visual symptoms of HFMD and is what makes this disease so recognizable. The rash on the hands typically appears around the same time as or shortly after the mouth sores.
- Appearance: Flat or slightly raised red spots or small blisters (vesicles) that may be surrounded by a red halo. They are typically oval or elongated in shape.
- Location: Most commonly found on the palms, but can also appear on the backs of the hands and between the fingers.
- Texture: The blisters may feel tender to the touch but are generally not itchy — this is an important distinguishing factor from conditions like chickenpox.
- Size: Sores are usually about 3 to 7mm in diameter.
- Healing: The blisters usually dry up and crust over within 7 to 10 days, leaving no permanent scarring in most cases.
6. Skin Rash on the Soles of the Feet
Alongside the hand rash, sores and blisters appear on the soles of the feet — the second major external site that gives the disease part of its name. The appearance is very similar to those on the hands.
- Location: Usually found on the soles, but may also appear on the tops of the feet and around the toes and ankles.
- Symptoms: Can cause pain or tenderness when walking or standing, which is why some children may limp or refuse to walk during the illness.
- Appearance: Red papules or blisters, similar in size and color to those on the hands.
- Not itchy: Like the hand rash, the foot rash is typically not itchy.
In mild early-stage hand, foot and mouth disease, the foot rash may only consist of a few flat red spots that can be easy to miss if not specifically looked for.
7. Rash on the Buttocks and Groin
Many parents and caregivers are surprised to learn that hand, foot and mouth disease can also cause a rash in areas beyond the hands, feet, and mouth. A rash on the buttocks, groin, and genital area is actually quite common, particularly in young children and infants in diapers.
- The rash in this area typically appears as flat red spots or small bumps rather than fluid-filled blisters.
- It may be mistaken for diaper rash in infants, so caregivers should check for other HFMD symptoms simultaneously.
- The rash is usually not painful or itchy in this location.
The presence of a buttocks rash alongside mouth sores and hand/foot blisters is a strong indicator that the illness is HFMD rather than another common childhood condition.
8. Rash on the Legs, Arms, and Body
In some cases — particularly in more severe infections or in adults — the rash can spread beyond the classic zones to affect the legs, arms, knees, elbows, and trunk (torso).
- This is more common when HFMD is caused by coxsackievirus A6, a strain associated with more widespread and more intense rashes.
- In adults, the rash may be more extensive and itchy compared to what is typically seen in children.
- In some cases, the blisters can be larger and more painful, resembling those of chickenpox.
When the rash becomes widespread, the condition can look more alarming, but it still usually resolves on its own within the standard recovery period.
9. Irritability and Malaise (General Feeling of Being Unwell)
Beyond the physical symptoms, HFMD causes a significant degree of irritability and general discomfort, especially in young children who cannot articulate how they are feeling.
- Children may be unusually fussy, clingy, or difficult to comfort.
- Sleep disturbances are common, as mouth pain can worsen when lying down.
- Older children and adults may describe feelings of fatigue, weakness, and general malaise — similar to how one feels at the onset of influenza.
- Headache and muscle aches may also be reported in some individuals.
10. Drooling (Especially in Infants and Toddlers)
Because the mouth sores are so painful, young children and infants with HFMD often drool excessively. This happens because swallowing is painful and children naturally reduce how often they swallow to avoid the discomfort.
- Excessive drooling is often one of the most noticeable early signs in babies and toddlers.
- It is frequently accompanied by refusal to eat, drink, or take a pacifier.
- This symptom is also an indicator of significant oral discomfort and should alert caregivers to check the inside of the child’s mouth for sores.
11. Nail Changes After Recovery
An often overlooked and lesser-known symptom — or rather, a post-illness sign — is changes to the fingernails and toenails that can occur weeks after recovering from HFMD.
- This condition is called onychomadesis, which refers to the temporary shedding or separation of nails from the nail bed.
- Nails may peel, split, or fall off entirely — which can be alarming but is generally harmless and temporary.
- New nail growth typically replaces the lost nails within a few months without any specific treatment.
- This side effect is more commonly reported following infections caused by coxsackievirus A6.
Parents should be reassured that nail loss following HFMD is a self-limiting complication, and the nails almost always grow back normally.
12. Dehydration (A Serious Complication to Watch For)
While not a symptom of HFMD itself, dehydration is one of the most serious complications that can arise from the illness, particularly in young children who refuse to drink due to painful mouth sores. It is critical to recognize the signs of dehydration early.
- Warning signs of dehydration include:
- Dry or sticky mouth
- No tears when crying
- Sunken eyes
- Significantly reduced urination (fewer wet diapers in infants)
- Unusual sleepiness or lack of energy
- Dry, cool skin
- If a child shows signs of dehydration, seek medical attention promptly.
- Offering cold fluids, ice chips, ice pops, or cold milk can help soothe the mouth and encourage fluid intake.
Main Causes of Hand, Foot and Mouth Disease
Understanding what causes HFMD helps in recognizing risk factors and taking steps to reduce transmission. The disease is caused by a group of viruses belonging to the Enterovirus genus.
- Coxsackievirus A16: The most common cause of HFMD in most parts of the world. It usually causes a mild illness.
- Coxsackievirus A6: Associated with more severe or widespread rash presentations, including more itching and larger blisters, and is more likely to cause nail shedding after recovery.
- Enterovirus 71 (EV-A71): A more serious strain that can, in rare cases, lead to neurological complications such as viral meningitis or encephalitis. More commonly reported in outbreaks across Asia.
- Other enteroviruses: Less commonly, other members of the enterovirus family can cause similar symptoms.
How it spreads:
- Direct contact with saliva, nasal discharge, blister fluid, or feces of an infected person
- Respiratory droplets from coughing or sneezing
- Touching contaminated surfaces and then touching the eyes, nose, or mouth
- Close personal contact such as hugging, kissing, or sharing utensils
HFMD is most contagious during the first week of illness, though the virus can remain in the body for weeks after symptoms resolve — meaning an infected person can still spread the virus even when they feel better.
Prevention of Hand, Foot and Mouth Disease
There is currently no vaccine available in most countries to prevent HFMD caused by coxsackievirus (though a vaccine against EV-A71 is available in some parts of Asia). The best defense is practicing consistent hygiene habits.
- Frequent handwashing: Wash hands thoroughly with soap and water for at least 20 seconds, especially after using the bathroom, changing diapers, and before eating.
- Avoid close contact: Keep infected children home from school or daycare until they are fever-free and all sores have healed to prevent spreading the illness to others.
- Disinfect surfaces: Regularly clean and disinfect frequently touched surfaces and objects such as toys, doorknobs, and countertops.
- Avoid sharing personal items: Do not share cups, utensils, towels, or toothbrushes with infected individuals.
- Respiratory hygiene: Cover coughs and sneezes with a tissue or the inside of the elbow, and dispose of tissues promptly.
- Avoid touching face: Reduce the habit of touching the eyes, nose, and mouth with unwashed hands.
Frequently Asked Questions (FAQ)
What does hand, foot and mouth disease look like?
HFMD typically presents with small red spots or blisters on the palms of the hands, soles of the feet, and painful ulcers inside the mouth. The rash may also appear on the buttocks and, in some cases, the arms, legs, and trunk. The sores are usually not itchy.
What are the early signs of hand, foot and mouth disease day by day?
Day 1–2: Fever, sore throat, and general feelings of being unwell (loss of appetite, irritability). Day 2–3: Painful sores begin to appear in the mouth. Day 3–5: The characteristic rash develops on the hands, feet, and possibly buttocks. Day 5–7: Symptoms typically begin to improve. Full recovery usually occurs within 7 to 10 days.
Can adults get hand, foot and mouth disease?
Yes. Although HFMD is most common in children under 5, adults can and do get infected — especially those who live with or care for young children. Adults may experience milder symptoms or, in some cases, a more widespread and itchy rash. Some adults may be infected and show no symptoms at all, yet still be contagious.
How long is HFMD contagious?
HFMD is most contagious during the first week of illness. However, the virus can continue to shed in feces for several weeks after symptoms have resolved, meaning an individual can still spread the virus even after feeling better.
Is hand, foot and mouth disease dangerous?
In the vast majority of cases, HFMD is a mild self-limiting illness that resolves on its own within 7 to 10 days. However, in rare cases — particularly with enterovirus 71 — serious complications such as viral meningitis, encephalitis, or myocarditis can occur. Seek immediate medical attention if the affected person develops a stiff neck, severe headache, difficulty breathing, or shows signs of dehydration.
How is HFMD different from chickenpox?
While both conditions cause blisters, there are key differences. HFMD blisters are located specifically on the hands, feet, and inside the mouth, and are generally not itchy. Chickenpox blisters appear all over the body, including the scalp, and are intensely itchy. A doctor can confirm the correct diagnosis if there is any doubt.
Should I see a doctor for hand, foot and mouth disease?
Most cases of HFMD can be managed at home with rest and supportive care. However, you should consult a doctor if: the fever is very high or lasts more than 5 days; symptoms are worsening; the child is showing signs of dehydration; or if neurological symptoms such as confusion, seizures, or severe headache appear. Always consult a healthcare professional before administering any medication.
References:
- Centers for Disease Control and Prevention (CDC) – Hand, Foot, and Mouth Disease
- World Health Organization (WHO) – Hand, Foot and Mouth Disease Fact Sheet
- Mayo Clinic – Hand, Foot and Mouth Disease: Symptoms and Causes
- NHS UK – Hand, Foot and Mouth Disease
- American Academy of Pediatrics (HealthyChildren.org) – Hand, Foot and Mouth Disease